Indicator 5: Emergency referral readiness
This indicator is defined as the proportion of facilities that meet an essential level of emergency referral readiness.
Numerator:No. facilities meeting the criteria for essential emergency referral readiness
Denominator:Total no. facilities assessed
× 100Purpose
With timely access to EmONC, most maternal and newborn deaths are preventable. However, reaching the right care at the right time remains a challenge for many women, particularly in low-income countries. Timely emergency referral between levels of the health system (i.e., interfacility referral) is widely acknowledged as a critical component of a high-quality health system – a required function that ensures women and newborns have access to definitive complication management. Yet, health planners and implementers often lack a comprehensive picture of how the interfacility emergency referral system is functioning, leaving them unable to systematically intervene to make improvements.
The emergency referral readiness indicator presented here provides health planners at the national and sub-national levels with an approach to monitor whether facilities have key elements in place to refer patients to a higher level of care. It is structured to enable targeted intervention by pinpointing where gaps exist. In addition, this indicator can support advocacy efforts to ensure the health system is functioning as it must to provide universal timely access to definitive lifesaving EmONC for the populations it serves.
The emergency referral readiness indicator focuses solely on interfacility referral, not on transport from home to facilities. We place focus here because the act of interfacility referral fits squarely within the health systems’ scope of responsibility and is a function that the majority of health facilities should be able to perform.
This indicator was developed through a consultative process over three years with pilot testing in limited settings. The composite indicator uses a scoring process that is similar to the scoring used in the Service Availability and Readiness Assessment and the Harmonized Health Facility Assessment.12
Data collection and calculation
The emergency referral readiness indicator is designed to be measured at the health facility level, among all facilities assessed. Data needed to calculate this indicator can be collected using the emergency referral readiness tool.
The emergency referral readiness indicator is a composite indicator comprised of six dimensions that encompass the different components of the interfacility referral system and are defined as follows:
- Transportation readiness: Describes a facility’s ability to quickly and effectively mobilize the necessary transportation for referral, including having ready access to a functional emergency vehicle that is maintained and appropriate for the local geography and climate.
- Referral efficiency & coordination of care: Refers to all that is needed to ensure that services for clients are efficiently and thoughtfully planned, communicated and executed across all care providers from first point of contact through definitive care. This includes the availability of explicit referral criteria and pre-referral stabilization guidelines.
- Care during transport: Encompasses the ability to offer continued quality care during referral, by having an appropriate provider with the skills, support, equipment and supplies needed, such that clients can remain stable throughout transfer.
- Financial accessibility of referral: Reflects the burden of costs that are borne by the client and their family related to the referral process or that affect the efficiency of the referral, as well as the health facility systems in place to minimize the financial burden of referral on clients.
- Family-centered referral: Comprises the components related to being able to offer thoughtful and respectful communication, inclusion, and consideration of families. This spans from the decision-making process regarding referral, through transfer and handover, with a prioritization on minimizing separation between caregivers and newborns and ensuring birth companionship.
- Inter-facility relational dynamics: Captures the interpersonal and organizational relationships, processes and tools across structures (i.e., levels of the health system) that affect the collaboration, coordination and care of referrals.
Variables within each of the six dimensions are organized into three levels of emergency referral readiness – essential, improved, and advanced – recognizing that different health systems and contexts may be at different points in establishing and strengthening their referral systems. The essential level captures the variables that are essential to a functional referral system. Response options that meet the essential level are indicated below in Table 1 and in the scoring framework. A health facility must meet all the criteria within the essential level to be classified as a facility with essential emergency referral readiness. Criteria and scoring for improved and advanced emergency referral readiness can also be found in the scoring framework as well as in Levels of emergency referral readiness: Criteria for essential, improved and advanced referral readiness.
Table 1: Criteria for essential emergency referral readiness
| Dimension | Criteria for essential emergency referral readiness |
|---|---|
| Transportation readiness | A health facility has access to at least one functional motor vehicle that is available 24/7, has sufficient fuel for transport and a driver. The vehicle can be either offsite or onsite. If offsite, it must be able to arrive in less than 30 minutes to the health facility. If vehicle is onsite, driver must be ready within 30 minutes at all times health facility offers services. Offsite vehicles are assumed to arrive with a driver. |
| Referral efficiency and coordination of care | A health facility has referral criteria,i referral guidelines/standard operating procedure/protocols,ii pre-referral management guidelinesiii and a policy to call ahead to receiving facilities as well as at least one form of communication that is free or supported by the health facility. |
| Care during transport | A health facility has a policy that patients being referred are accompanied by a provider, typically practices accompaniment by a provider, the providers have the skills to perform key emergency maternal and newborn clinical tasks and the equipment to do so. Further, providers are trained in how to transfer small and sick newborns and typically transfer newborns in KMC position, incubator or radiant warmer. |
| Financial accessibility of referral | A health facility ensures costs related to services or transport do not delay referral. |
| Family-centered referral | A health facility has policies in place to allow at least one family member/caregiver or birth companion to accompany a patient during referral. |
| Inter-facility relational dynamics | A health facility has, at minimum, a directoryiv of facilities and a policy requiring staff to confirm receiving facility capacity prior to referral. |
i. Referral criteria are a set of evidence-based guidelines for clinicians to determine when a patient needs to be referred to a higher level of care, typically based on facility level capacity, the severity of a patient’s condition and likelihood of the condition worsening.
ii. Referral guidelines, standard operating procedures or protocols refer to a predefined set of steps to carry out an emergency referral.
iii. Pre-referral management guidelines are the clinical guidelines to manage emergency conditions and stabilize patients prior to referral.
iv. A directory is a list of organizations or facilities that provide obstetric and newborn care, and other related services, in the area. It should typically include contact information for all services at the facilities as well as their location and hours of operation.
The numerator for this indicator is calculated by summing the number of facilities that are classified as having at least essential referral readiness.3
The denominator refers to all health facilities being assessed.
The emergency referral readiness indicator is typically expressed as a percentage.
Data are ideally collected at the end of every quarter or 6-month period using the emergency referral readiness tool, either by facility staff as part of HMIS or program reporting or by an external assessment team interviewing staff.
Analysis and interpretation
The benchmark for this indicator is 100%, such that all health facilities should aim to achieve at least an essential level of referral readiness. If a country has less than 100%, then the health system has not fulfilled its responsibility to ensure that clients requiring emergency interfacility referral can reach definitive treatment within an appropriate amount of time.
Disaggregation by geographic area, level of facility, EmONC classification, and/or managing authority may uncover systemic problems in referral readiness.
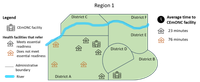
The indicator can also be stratified by time or distance to nearest health facility with surgical capacity. Health facilities that are farther away from facilities offering Comprehensive EmONC services will result in longer and potentially more difficult journeys for clients to reach definitive care. As the referral time increases, the need for more consistent and substantial care during transport also increases to ensure clients can remain stable throughout transfer. For example, while a short journey may not require extensive clinical support, on a longer journey there is a higher likelihood that a client will need continuous clinical monitoring and management to prevent a decline in health condition to enable surgery, receive a blood transfusion or receive respiratory support, as needed. Mapping facilities by referral readiness can help visualize disparities in readiness by distance and geography. Figure 1 demonstrates how a rudimentary mapping can quickly communicate the need to improve referral readiness in the health facilities furthest away from the District A or District B hospitals.
Figure 1: Map of Region 1, plotting health facilities in District A by emergency referral readiness classification in hypothetical country
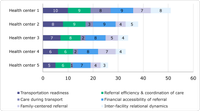
Referral readiness scores can also be disaggregated and calculated for each dimension using the scoring framework so health planners can identify what components of the referral system need strengthening. This information can either be analyzed at an aggregated level (i.e., calculating average dimension scores across facilities to identify systemic gaps) or at a facility level. For example, in Figure 2, data for five imaginary health centers within a district are presented with their emergency referral readiness scores broken down by dimension. In this example, each dimension is scored out of 10 for a possible total of 60 points. Note that no health center has achieved essential emergency referral readiness (or a total score of 60 points) during this reporting period. Using a stacked bar chart, it becomes clear that Health Center 1 is most ready to refer, whereas Health Center 5 needs more support. This visual also highlights that health facilities within this district tend to be weaker in the areas of care during transport and inter-facility dynamics whereas they are strong in financial accessibility. It is recommended to further explore the individual variables within each dimension to inform targeted action plans.
Figure 2: [Designated Basic EmONC (BEmONC)] Health center emergency referral readiness scores, by dimension in hypothetical country
Lastly, emergency referral readiness can be examined with other indicators that capture additional aspects of the EmONC referral system. For example, Indicator 6 Home to Comprehensive EmONC within 1 hour estimates the population’s timely access to Comprehensive EmONC from home. The referral signal function (arrange ambulance, with trained and equipped provider, to a facility that can provide definitive care) provides information about whether facilities have actually executed a referral that included continued clinical care during interfacility transfer at least once in the last three months.
Supplemental studies
In addition to facility level readiness, it is important for health planners to measure how the interfacility referral system is functioning, and whether it is efficient or impactful. Below we offer suggestions for supplementary studies that address those processes and outcomes.
Referral volume
It may be helpful to analyze referral readiness together with referral volume. (The data needed for a referral volume analysis would already be collected if a country decides to calculate the ‘direct obstetric complications referral rate,’ listed as a supplemental study under Indicator 8: Met need for emergency obstetric care.) Facilities can be grouped based on their referral volume, and then disaggregated by their level of emergency referral readiness. Comparing referral readiness levels of health facilities that refer a large number of obstetric and neonatal emergencies to those that refer a small number can highlight where system upgrades can serve the greatest number of clients.
Referral system functionality
Measures of referral efficiency are of high interest to health planners and researchers; however, they are challenging to collect because they typically require patient-level data from more than one location, which are often not available within routine health systems data sources. Thus, these efficiency measures will require special studies. They are most useful if benchmarks exist for comparison. Examples include:
- Time intervals: Time from ‘decision to refer’ to ‘patient leaving referring site’ (example benchmark: under 30 minutes); time to transfer patient to more advanced care (example benchmark: under 30 minutes); total time from ‘decision to refer’ to ‘definitive treatment’ (example benchmark: under 60 minutes).
- Number of stops along the journey: This can provide insight into the efficiency/inefficiency of the referral system, specifically of interfacility relational dynamics and coordination of care, i.e., whether facilities are able to communicate and to coordinate referral in real time. In contexts where a centralized ambulance system and dispatch system is in place (e.g., India), it may be possible to calculate this by analyzing data that are routinely collected through that system. However, in most LMICs, this would require a special study.
Outcomes among referred patients
Ideally, one would be able to relate referral system readiness and/or functioning to health outcomes among referred patients. In places where referral registers are kept at sending and receiving facilities, this may be possible through an audit process. Example indicators that could be analyzed from typical referral register data include:
- Condition of patient upon arrival can provide insight into the functionality of the referral system, for example: presence or onset of specific conditions (e.g., hypothermia, hypoxia, apnea, hypotension); number/incidence of unresponsive patients upon arrival; and need for cardiorespiratory support immediately upon arrival. For newborns, it may be useful to capture incidence of hypoglycemia upon arrival, and of hypothermia and hypoxia upon arrival without an on-going intervention.
- Mortality rates among referred patients: aggregate measure of mortality at receiving facilities among obstetric cases received, and among newborns received. Depending upon the volume of referrals, the mortality rates could be further disaggregated by sending facility and potentially correlated with facility readiness score. Further, the timing of any death could provide insight into the presence of care during transport and/or the sending facilities’ ability to rapidly mobilize for interfacility referral. Example indicators include: the frequency of death during transport, and of deaths within a specific timeframe after arrival at receiving facility (e.g., 1-2 hours). Interpretation of changes in this rate will vary in relation to referring facility capacity, service delivery and referral practices.
Useful links
Facility-level assessment of signal function readiness and referral (Ghana paper: https://pubmed.ncbi.nlm.nih.gov/30777082/)
Service Availability and Readiness Assessment (SARA). An annual monitoring system for service delivery. Reference Manual. (2015) World Health Organization. ↩︎
Harmonized health facility assessment (HHFA): comprehensive guide. (2022) World Health Organization. ↩︎
In contexts where referral systems are well-established and most health facilities already meet the essential level of referral readiness, a government may choose to change the numerator to the number of facilities that achieve the improved or advanced readiness levels instead of the essential level. ↩︎