What’s new in the EmONC Framework?
“Re-visioning EmONC”: Review, rethink, revise
The 1997 and 2009 emergency obstetric care frameworks used available facility-level data to enable countries to generate a rough estimate of availability, accessibility, use and quality of their services. As part of the “Re-visioning EmONC” initiative, the project team undertook to review, rethink and revise this framework. The project examined available literature on the EmONC Framework elements (signal functions, levels of care, and indicators), including both studies using the Framework and commentaries critiquing it. The project also did multiple analyses of the data sets available from national EmONC assessments done over the years. Using human-centered design methods, the project conducted country studies in Malawi, Senegal and Bangladesh. It also organized a Delphi survey and consulted very widely with users of the Framework as well as experts in the MNH field. (Figure 1) The Re-Visioning EmONC process and evidence base for revised EmONC Framework provides details on the project’s process and the evidence base it developed.
Figure 1: Human-centered approach to Re-Visioning EmONC
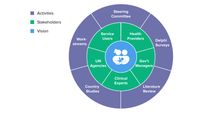
The revised EmONC Framework aligns with norms developed through formal WHO processes, including clinical norms and health systems norms. Recently issued norms for the care of small and sick newborns have been integrated into this guide.1 Forthcoming norms for maternal health will be integrated as soon as they are issued.
10 key changes in the EmONC Framework
Several important conclusions from those activities inform the new vision of EmONC put forward in this Guide:
-
EmONC as a system:
Too often in the past, EmONC has been understood and addressed as simply a collection of discrete clinical interventions or even just a set of clinical signal functions, for treating maternal and newborn complications. But to deliver equitable, good quality care across a population – especially a heterogenous population of different racial/ethnic groups, rural/urban communities, varying socioeconomic and citizenship status – EmONC must also be understood as a system. A system has many interlinked, interdependent components, that must all function together to meet the goal: right care in the right place at the right time.
The updated set of indicators provided in this framework captures more fully the systems components needed for EmONC to function optimally. These are divided conceptually into structure, process and outcome indicators. They highlight several aspects of system functioning that are especially important to EmONC, including a ready and reliable supply of specific commodities, an efficient emergency referral system, and a sufficient number of trained and competent professionals for facilities to meet the workload and to function 24 hours a day, 7 days a week. The new indicator set also recognizes that, even in a life-threatening emergency, people are making choices: women and families are deciding how and where to engage with the health system, and health providers are deciding how those women and newborns will be received and managed. The social, psychological and physical environments in which these decisions are made matter greatly to the way that people experience the health care system and to the outcomes it produces.2 Fundamental human rights demand respectful care for patients and a decent, supportive workplace for providers. People-centeredness is an important characteristic of a well-functioning system and is now better captured by the new indicator set.
The EmONC Guide supports planners and managers to address each key part of the EmONC system and to see it as a functioning whole. At the same time, that EmONC system is embedded in a country’s broader health system, not separate from it. This means that meaningful change in some components of EmONC, such as the procurement system for drugs and equipment or the referral system for inter-facility transfer, must be coordinated with overall health system reforms addressing these issues. And, conversely, health planners responsible for these sub-systems, such as procurement, need to be alert to the specific requirements for providing effective, good quality EmONC.
-
Integration into planning processes:
The Guide envisions a different process for assessing, planning and monitoring EmONC than used in the past. The previous versions of this Guide identified a simple set of availability, accessibility and utilization indicators, but did not link them directly to overall government planning processes. Many countries have conducted occasional, large, national EmONC assessments using detailed data collection modules developed by Columbia University/AMDD, but only when external funding was available to support it – typically not more than every 5 to 10 years. This Guide proposes that, as much as possible, indicators be explicitly built into country planning and monitoring processes, so that they are tracked systematically and analyzed at regular intervals that support long-term (±10 year) strategic planning processes, as well as 3-5 year programme cycles, with a small subset used annually, semi-annually or quarterly for ongoing monitoring of system functioning. The process builds on the EmONC implementation guide developed by UNFPA and the countries where it has been implemented in Sub-Saharan Africa and Southeast Asia.
The Guide explicitly considers the need to adapt the EmONC Framework to the country’s existing system. Adaptation is to ensure that planning processes begin by assessing the country’s existing systems, structures, and needs – and, from that starting point, build a strong, locally-driven vision about where the country will go and how it will get there. Guidance about how to adapt the EmONC Framework is integrated throughout the Guide.
-
Newborn care:
The 1997 edition of the Handbook addressed only obstetric complications; in 2009 one signal function on newborn resuscitation was added. Studies of newborn mortality and stillbirths, including causes of death and projected impact of interventions, have made it clear that emergency obstetric care has significant impact on newborns as well as women.3 Moreover, with high levels of institutional delivery, and other technical advances, the newborn field has pivoted from home-based newborn care to focus on facility-based care for the small or sick newborn, including the creation of special newborn care units (SNCUs) and newborn intensive care units (NICUs) in facilities.45 A major change in the revised EmONC Framework and Guide is the full inclusion of care for small or sick newborns. The term “emergency obstetric care” (EmOC) has been changed to “emergency obstetric and newborn care” (EmONC).
-
Levels of EmONC:
With the incorporation of care for small and/or sick newborns, the project reviewed and revised the levels of care used to assess EmONC. The 1997 and 2009 Handbook, which focused only on obstetric complications, defined two levels of emergency obstetric care, Basic and Comprehensive, with the capacity to perform surgery and blood transfusion at the comprehensive level as the key distinction between them. On the newborn side, WHO/UNICEF’s 2019 “Survive and Thrive: Transforming care for every small and sick newborn” described multiple levels of care, including a level of intensive care provided in major teaching hospitals. The Re-visioning EmONC project conducted a systematic review to determine the most common configuration of levels of care used in health systems and proposed, for both obstetric and neonatal complications, a 3-level EmONC model: Basic, Comprehensive and Intensive EmONC.
-
Availability benchmark:
The benchmark for availability in the initial 1997 EmOC Framework was 4 Basic EmOC and 1 Comprehensive EmOC facility per 500,000 population. In 2009, this was modified to 5 EmOC facilities, at least one of which is Comprehensive, per 500,000 population. This benchmark was based on multiple assumptions: First, the choice of 5 EmOC facilities per 500,000 population was based on an estimate of the number of obstetric complications likely to occur in that population, and the proportion of those complications that would require surgery or blood transfusion, only available in Comprehensive EmOC facilities. With a rough sense of the number of complications that could typically be managed in health centers and hospitals in high mortality countries, the previous frameworks set a benchmark assuming that, at a minimum, EmONC facilities would be needed to treat complications. Routine deliveries would take place largely in lower-level facilities or at home, as was the case at the time, and women who experienced complications would be transferred to facilities providing Basic or Comprehensive EmONC. But in 2024, institutional delivery rates are far higher - in 46 low and lower middle income countries institutional delivery rates have risen steadily from an average of 44% between 2000-2005 to 77% in 2017-2022.6 At the same time, many women are bypassing lower level facilities to give birth at higher level facilities.789 Planners cannot assume that EmONC facilities are only treating mothers with complications; they are typically conducting many normal deliveries as well.
Second, the denominator of 500,000 population was intended to capture 20,000 births, by assuming an average crude birth rate of 40 in a population of 500,000. But that assumption became increasingly unjustified as fertility rates changed and varied across countries. In the revised Framework, countries are encouraged to use their local crude birth rate to factor into the calculation of how many facilities are needed.
Third, recommending a universal benchmark for all countries implicitly assumes that facilities in different countries have similar caseload capacities. But analysis of assessment data shows that EmONC facility size can vary dramatically within a country and from one country to another.
Fourth, the earlier editions of the EmONC Handbook insisted that all women have access to emergency obstetric care in case of a complication, but they were implicitly agnostic about where women gave birth. But exactly where – what kind of facility – women give birth in matters. How many births take place in low volume facilities (<600 births per year) versus high volume facilities varies from country to country. For example, in Malawi in 2020 51% of facilities would be considered low volume facilities but only 17% of the facility births occurred in those facilities; whereas in Zambia in 2014, 72% of facilities would be considered low volume and accounted for 40% of facility births (unpublished EmONC assessment data).
Unpublished assessment data suggest that on average, it takes a median of 53 deliveries per month for non-hospitals to perform 6 of the Basic EmONC maternal signal functions (parenteral antibiotics, uterotonic drugs, parenteral anticonvulsants, manually remove placenta, remove retained products, and perform assisted vaginal birth) over a 3-month period. This suggests that low volume facilities (i.e., those with <600 births per year) will have challenges performing and sustaining EmONC. (See Re-Visioning EmONC process and evidence base for revised EmONC Framework.)
In 2024, there is growing consensus that all women should give birth at a facility that can provide, at minimum, Basic EmONC and be in close proximity to a Comprehensive EmONC facility with referral linkages to Intensive EmONC facilities.10 The revised approach to the availability indicator and benchmark reflects this consensus, as well as the fact that countries’ health systems and childbirth patterns are increasingly different. As described in the section titled ‘How to use the EmONC Framework’ and in the sections describing indicators 1a and 1b, the revised Framework guides countries in setting their own availability benchmark in a two-step process to inform first a long-term goal of having enough EmONC facilities for all women and newborns, and then setting interim benchmarks over 3-5 year programme planning cycles, taking into account multiple factors including the average size of facilities (i.e., number of delivery beds), availability of human resources, equity and geographic access.
-
Signal functions:
Signal functions are a parsimonious list of clinical tracer interventions, representing key processes of care, to treat the main complications of childbirth that would otherwise result in maternal or newborn death and disability, or stillbirth (see EmONC Signal Functions). The Re-visioning EmONC project conducted a narrative review of the literature on the use of signal functions11 as well as a Delphi study, and engaged in multiple discussions of the issue both inside and outside the project. Given the strong opinions in their favor, and their successful use in dozens of assessments and monitoring projects to guide planning, it was decided that signal functions would continue to be the grounding for this Framework.
The revised Framework contains an updated set of agreed signal functions that now include: tracer interventions for the care of small and sick newborns, a signal function on emergency referral, and tracer interventions for intensive care. To enhance the precision and reliability of measuring certain existing signal functions, some have been re-named (e.g., “administer uterotonic drugs” is now “administer medications to treat post-partum hemorrhage”; “administer parenteral anticonvulsants for pre-eclampsia and eclampsia” is now “administer magnesium sulfate”).
-
Readiness:
While the original Framework had the virtue of simplicity, it proved to be too simple. For example, it measured the performance of signal functions, and assumed that if a signal function was performed, the facility had the basic technical inputs – human resources, drugs, equipment – to do that signal function 24h/7d. Data and experience show that this assumption is not warranted. The revised Framework therefore includes indicators of “readiness” or “structure”, touching on major areas needed for implementing EmONC at the facility level, including infrastructure, commodities, human resources adequacy, and emergency referral readiness.
-
Human resources:
Perhaps the most important aspect of readiness that was assumed, but not measured, in the previous Framework was human resources. Even where facilities did perform signal functions, more detailed assessments very often showed too few staff, too poorly trained, and working under such difficult conditions that consistent, sustained good quality care was unlikely or impossible. Deficient health system planning and financing leave health providers on the frontline responsible for grappling with system failures; when the dysfunction cannot be overcome, provider wellbeing and performance is impacted.1213 In short, the supply, competency and wellbeing of health workers affect – and are affected by – almost every aspect of facility functioning. The need – indeed, the demand – for measures to address human resource challenges was perhaps the #1 finding from the country studies. The revised Framework adds measures on human resource adequacy per shift for caseload (Indicator 4) and workforce wellbeing (Indicator 12).
-
Quality of care:
The original 1997 Framework had one simple measure, the direct obstetric case fatality rate, to give a rough sense of quality of care. In 2009, the indicator “intrapartum and very early neonatal death rate”14 was added, with the reasoning that good quality intrapartum care could save many babies who died during delivery and were recorded as either stillbirths or very early neonatal deaths (within the first 24 hours). But the last 15 years have seen huge steps in the quality of care field, including the rise of the respectful care movement,15 new methods of quality improvement implemented on the ground and supported by global networks,16 as well as major attention to quality of care measurement in multilateral agencies.17 The revised Framework integrates quality of care measures in multiple parts of the Framework, including readiness and appropriateness of care indicators, aligning where possible with global quality of care initiatives. It also includes measures of experience of care of both mothers and newborns. These are each described separately (see EmONC Indicators) and then brought together in one section on quality of care (Exploring quality of care with the EmONC Indicators) that integrates the different measures to give the user an overall picture of how the Framework helps planners to flag specific quality of care problems for further action.
-
Emergency referral systems:
Although it was well understood that many women would need emergency referral, the previous Framework itself had no measures of referral processes or connections between Basic and Comprehensive EmONC facilities. With improvements in road networks, innovative ambulance and dispatch systems, and more attention to networks of care approaches, the potential for a good referral system to save many lives is within reach. The revised Framework includes multiple points of attention to emergency referral: a new signal function at the Basic EmONC facility level; and an index of emergency referral readiness.
Together, these changes represent an expansion of the previous 2009 Framework, inspired by the adage: “Everything should be as simple as possible, but not simpler.” Some indicators have been used for decades with only minor adjustments recommended here; others are new, proposed to fill critical identified gaps (such as human resources), and will be validated in use in the coming years. We include them in the EmONC Framework and Guide, with appropriate caution that their validity as measures is still to be confirmed, because it is impossible – even deceptive – to try to build a picture of how the EmONC system is functioning without them.
Forthcoming. ↩︎
WHO. WHO recommendations: intrapartum care for a positive childbirth experience. Geneva: World Health Organization; 2018. Licence: CC BY-NC-SA 3.0 IGO. ↩︎
Bhutta, Z. A., Das, J. K., Bahl, R., Lawn, J. E., Salam, R. A., Paul, V. K., Sankar, M. J., Blencowe, H., Rizvi, A., Chou, V. B., Walker, N., Lancet Newborn Interventions Review Group, & Lancet Every Newborn Study Group (2014). Can available interventions end preventable deaths in mothers, newborn babies, and stillbirths, and at what cost?. Lancet (London, England), 384(9940), 347–370. ↩︎
WHO. Standards for improving quality of care for small and sick newborns in health facilities. Geneva: World Health Organization; 2020. Licence: CC BY-NC-SA 3.0 IGO. ↩︎
WHO. Survive and thrive: transforming care for every small and sick newborn. Geneva: World Health Organization; 2019. Licence: CC BY-NC-SA 3.0 IGO. ↩︎
Analysis of Multiple Indicator Cluster Survey (MICS) data and Demographic and Health Survey (DHS) data downloaded from https://mics.unicef.org/surveys and https://www.statcompiler.com/en/; accessed on 9 June 2024. ↩︎
Amoro, V. A., Abiiro, G. A., & Alatinga, K. A. (2021). Bypassing primary healthcare facilities for maternal healthcare in North West Ghana: socio-economic correlates and financial implications. BMC health services research, 21(1), 545. ↩︎
Maharjan, M., Sharma, S., & Kaphle, H. P. (2024). Factors associated with bypassing primary healthcare facilities for childbirth among women in Devchuli municipality of Nepal. PloS one, 19(4), e0302372. ↩︎
Mubiri, P., Kajjo, D., Okuga, M., Marchant, T., Peterson, S., Waiswa, P., & Hanson, C. (2020). Bypassing or successful referral? A population-based study of reasons why women travel far for childbirth in Eastern Uganda. BMC pregnancy and childbirth, 20(1), 497. ↩︎
Forthcoming. ↩︎
Moxon, S. G., B, S. S., Penn-Kekana, L., Sharma, S., Talbott, J., Campbell, O. M. R., & Freedman, L. (2024). Evolving narratives on signal functions for monitoring maternal and newborn health services: A meta-narrative inspired review. Social science & medicine (1982), 352, 116980. Advance online publication. ↩︎
Ramsey, K. (2022). Systems on the edge: developing organizational theory for the persistence of mistreatment in childbirth. Health Policy and Planning 37(3): 400-415. ↩︎
Reddy, B., Thomas, S., et al. (2022). A scoping review of the impact of organizational factors on providers and related intervention in LMICs: Implications for respectful maternity care. PLOS Global Public Health. ↩︎
Note that this indicator is still in the indicator set but its name has been slightly changed to: “intrapartum stillbirth and very early neonatal death rate.” ↩︎
Forthcoming. ↩︎
Forthcoming. ↩︎
Forthcoming. ↩︎